What is Eczema (Atopic Dermatitis)?
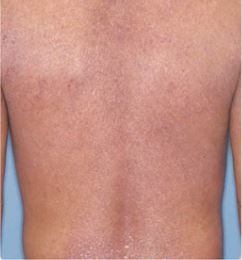
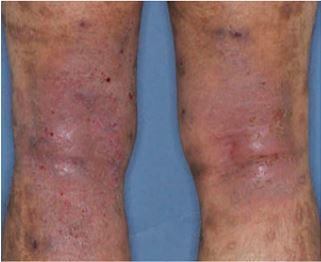
Eczema (Atopic dermatitis) is a condition in which one suffers from itchiness and repetitive red skin rashes. Eczema is a chronic (continuous) inflammatory skin condition with fluctuating symptom intensity.
In the majority of cases, skin symptoms appear in infancy or childhood, but late onset in adolescence and adulthood can also occur. In general it is less prevalent with age.
Eczema may accompany other allergic conditions such as asthma, allergic rhinitis, and allergic conjunctivitis. These conditions may develop in blood relatives. Eczema has a tendency to produce higher levels of IgE, an antibody related to allergies.
In the majority of cases, skin symptoms appear in infancy or childhood, but late onset in adolescence and adulthood can also occur. In general it is less prevalent with age.
Eczema may accompany other allergic conditions such as asthma, allergic rhinitis, and allergic conjunctivitis. These conditions may develop in blood relatives. Eczema has a tendency to produce higher levels of IgE, an antibody related to allergies.
|
|
One Way To Understand The Development Of Eczema (Atopic Dermatitis)
One model to understand the development of atopic dermatitis (and its clinical varieties) can be explained by the complexity of the interplay among (1) skin barrier dysfunction, (2) immunological response, and (3) pruritus (itchiness) (Figure 1). These factors are closely related to each other and also contribute to the chronicity of the disease. Let’s take a closer look at each factor one by one. This is going to get a little technical.
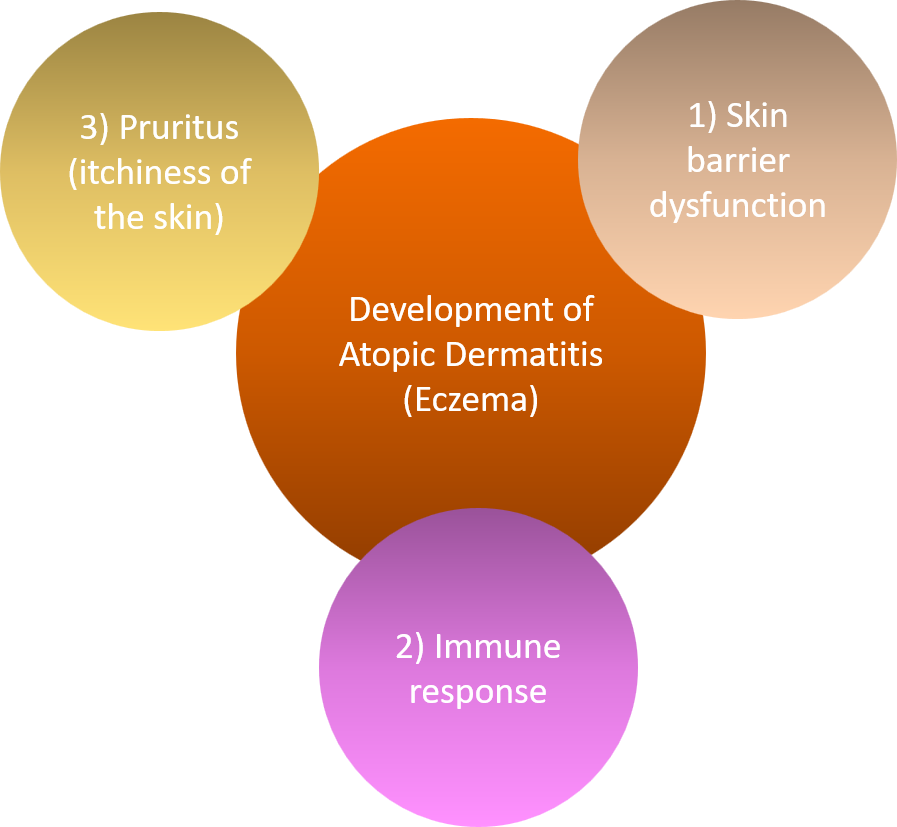
1) Kabashima K. J Dermatol sci 70: 3-11, 2013
1) Skin barrier dysfunction
Figure 2 shows normal epidermis vs. epidermis with skin barrier dysfunction. The uppermost layer of the epidermis is called stratum corneum and it functions as ‘a barrier.’ It prevents excessive water loss from inside the body as well as the invasion of any external pathogens or allergens. In eczema (atopic dermatitis), this skin barrier does not operate properly, increasing one’s susceptibility to external non-specific and specific stimuli, leading to skin inflammation (an immune response). Also, the study has shown that a substance called ‘filaggrin,’ the source of so-called ‘natural moisturizing factor’ in the stratum corneum and ‘ceramide,’ a substance also important in the moisture and protection in the skin barrier are scarce in patients with eczema (in the case of filaggrin scarcity, it can be due to genetic factors).
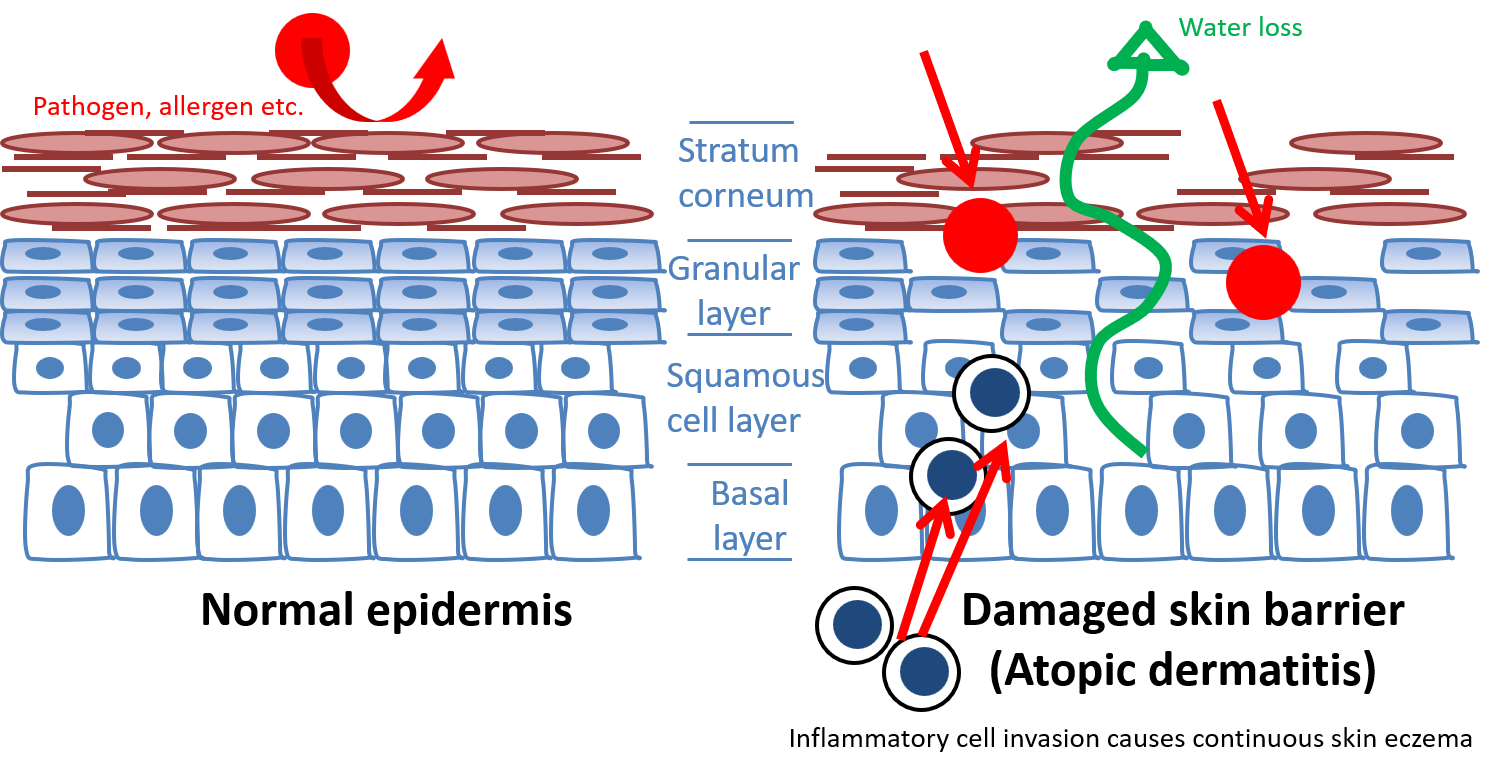
Figure 2. Normal epidermis vs. epidermis with damaged skin barrier in eczema
2) Immune response
Immune response, or immune cell reaction, in eczema has both the aspects of so called ‘innate immunity’ and ‘adaptive immunity.’
In innate immunity, the immune response is caused by non-specific external pathogens (such as bacteria, viruses, and parasites), which provoke immune reactions in almost the same manner. Innate immunity is an immune mechanism that you are born with.
On the other hand, in adaptive immunity there is a specific immune response; where immune cells memorize and react to specific pathogens such as house dust mites. Adaptive immunity is an immune mechanism that one develops over time.
In innate immunity, the immune response is caused by non-specific external pathogens (such as bacteria, viruses, and parasites), which provoke immune reactions in almost the same manner. Innate immunity is an immune mechanism that you are born with.
On the other hand, in adaptive immunity there is a specific immune response; where immune cells memorize and react to specific pathogens such as house dust mites. Adaptive immunity is an immune mechanism that one develops over time.
3) itchiness of the skin
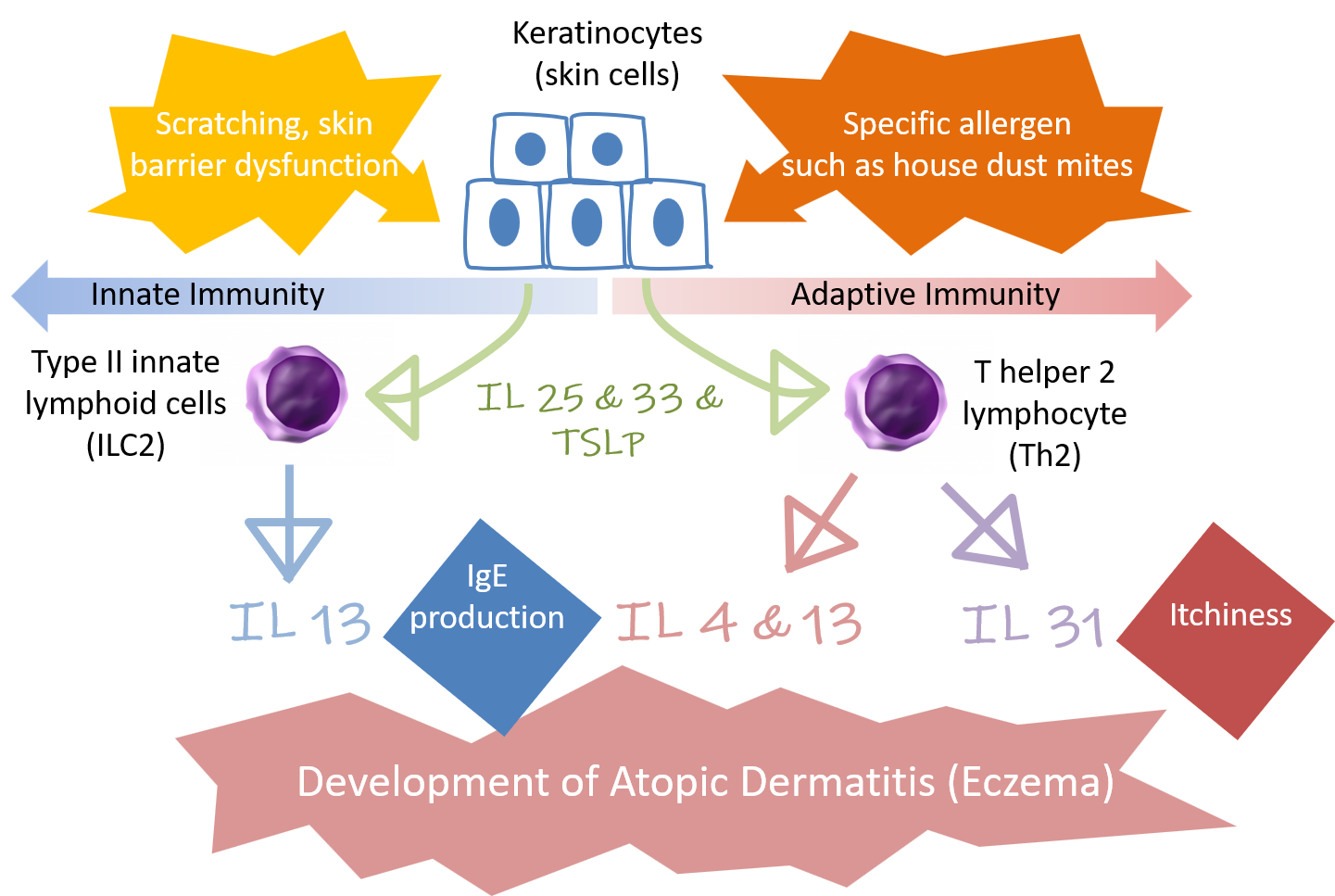
When you scratch the itchy skin, the external pathogens come in contact with the keratinocyte (the most predominant skin cell), it produces substances (such as IL25, IL33, and TSLP).
These substances stimulate type II innate lymphoid cells (ICL2) (which usually is deployed in innate immunity) and T helper 2 lymphocytes (Th2) (which, by contrast, is involved in adaptive immunity) causing ICL2 to secrete IL13, and Th2 to secrete IL4, IL13, IL31, which are key molecules in the development of eczema.
IL4 and IL13, as a result, increase the production of IgE, an antibody related to allergies. And IL31 is thought to cause itchiness by directly stimulating the nerve endings (Figure 3).
These substances stimulate type II innate lymphoid cells (ICL2) (which usually is deployed in innate immunity) and T helper 2 lymphocytes (Th2) (which, by contrast, is involved in adaptive immunity) causing ICL2 to secrete IL13, and Th2 to secrete IL4, IL13, IL31, which are key molecules in the development of eczema.
IL4 and IL13, as a result, increase the production of IgE, an antibody related to allergies. And IL31 is thought to cause itchiness by directly stimulating the nerve endings (Figure 3).
Self-Evaluation Tools for Eczema (Atopic Dermatitis)
Here are useful questionnaires to know the extent of, and the control status of eczema over the past week. They are POEM and ADCT.
POEM (The Patient Oriented Eczema Measure)
In POEM (Patient Oriented Eczema Measure), the patient or patient’s parents can assess the severity of the eczema (atopic dermatitis) over the past week by answering the questionnaire.
POEM questionnaire consists of seven questions regarding major symptoms of eczema, and it assesses the extent of eczema by adding the scores of each item. Higher scores might indicate the severity of the symptoms. The maximum score is 28 points.
POEM questionnaire consists of seven questions regarding major symptoms of eczema, and it assesses the extent of eczema by adding the scores of each item. Higher scores might indicate the severity of the symptoms. The maximum score is 28 points.
1. Over the last week, on how many days has your skin been itchy because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
2. Over the last week, on how many nights has your sleep been disturbed because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
3. Over the last week, on how many days has your skin been bleeding because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
4. Over the last week, on how many days has your skin been weeping or oozing clear fluid because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
5. Over the last week, on how many days has your skin been cracked because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
6. Over the last week, on how many days has your skin been flaking off because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
7. Over the last week, on how many days has your skin felt dry or rough because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
What does a POEM total score mean?
-Clear or almost clear = 0 to 2;
-Mild eczema = 3 to 7
-Moderate eczema = 8 to 16
-Severe eczema = 17 to 24;
-Very severe = 25 to 28
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
2. Over the last week, on how many nights has your sleep been disturbed because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
3. Over the last week, on how many days has your skin been bleeding because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
4. Over the last week, on how many days has your skin been weeping or oozing clear fluid because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
5. Over the last week, on how many days has your skin been cracked because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
6. Over the last week, on how many days has your skin been flaking off because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
7. Over the last week, on how many days has your skin felt dry or rough because of the eczema?
□ No days (0 points)
□ 1-2 days (1 point)
□ 3-4 days (2 points)
□ 5-6 days (3 points)
□ Every day (4 points)
What does a POEM total score mean?
-Clear or almost clear = 0 to 2;
-Mild eczema = 3 to 7
-Moderate eczema = 8 to 16
-Severe eczema = 17 to 24;
-Very severe = 25 to 28
Charman CR et al. Arch Dermatol. 2004: 140: 1513-1519
ADCT (Atopic Dermatitis Control Tool)
There is also a questionnaire called ADCT (Atopic Dermatitis Control Tool) that allows patients to assess the efficacy of the treatment in the past week.
ADCT questionnaire consists of six questions regarding major symptoms of the eczema, and it assesses the extent of eczema by adding the scores of each item.
A high score might indicate a worsening condition for the past week. The maximum score is 24 points.
ADCT questionnaire consists of six questions regarding major symptoms of the eczema, and it assesses the extent of eczema by adding the scores of each item.
A high score might indicate a worsening condition for the past week. The maximum score is 24 points.
1. Over the last week, how would you rate your eczema-related symptoms (for example, itching, dry skin, skin rash)?
□ None (0 points)
□ Mild (1 point)
□ Moderate (2 points)
□ Severe (3 points)
□ Very severe (4 points)
2. Over the last week, how many days did you have intense episodes of itching because of your eczema?
□ Not at all (0 points)
□ 1 to 2 days (1 point)
□ 3 to 4 days (2 points)
□ 5 to 6 days (3 points)
□ Every day (4 points)
3. Over the last week, how bothered have you been by your eczema?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
4. Over the last week, how many nights did you have trouble falling or staying asleep because of your eczema?
□ Not nights (0 points)
□ 1 to 2 nights (1 point)
□ 3 to 4 nights (2 points)
□ 5 to 6 nights (3 points)
□ Every night (4 points)
5. Over the last week, how much did your eczema affect your daily activities?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
6. Over the last week, how much did your eczema affect your mood or emotions?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
A patient’s atopic dermatitis may not be adequately controlled if:
-Their ADCT total score is at least 7 points
OR
-Their ADCT total score increased by 5 points or more since they last used ADCT
□ None (0 points)
□ Mild (1 point)
□ Moderate (2 points)
□ Severe (3 points)
□ Very severe (4 points)
2. Over the last week, how many days did you have intense episodes of itching because of your eczema?
□ Not at all (0 points)
□ 1 to 2 days (1 point)
□ 3 to 4 days (2 points)
□ 5 to 6 days (3 points)
□ Every day (4 points)
3. Over the last week, how bothered have you been by your eczema?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
4. Over the last week, how many nights did you have trouble falling or staying asleep because of your eczema?
□ Not nights (0 points)
□ 1 to 2 nights (1 point)
□ 3 to 4 nights (2 points)
□ 5 to 6 nights (3 points)
□ Every night (4 points)
5. Over the last week, how much did your eczema affect your daily activities?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
6. Over the last week, how much did your eczema affect your mood or emotions?
□ Not at all (0 points)
□ A little (1 point)
□ Moderately (2 points)
□ Very (3 points)
□ Extremely (4 points)
A patient’s atopic dermatitis may not be adequately controlled if:
-Their ADCT total score is at least 7 points
OR
-Their ADCT total score increased by 5 points or more since they last used ADCT
David M Pariser et al. Curr Med Res Opin. 2020: 36: 367-376
Treatment of eczema (atopic dermatitis)
Since eczema repeatedly causes skin inflammation and requires a long treatment course. The treatment is directed towards alleviating the ongoing symptoms. One needs to continue the treatment, with the goal of maintaining a condition that is virtually symptom-free, or if present, minor, and does not interfere with patients’ daily activities.
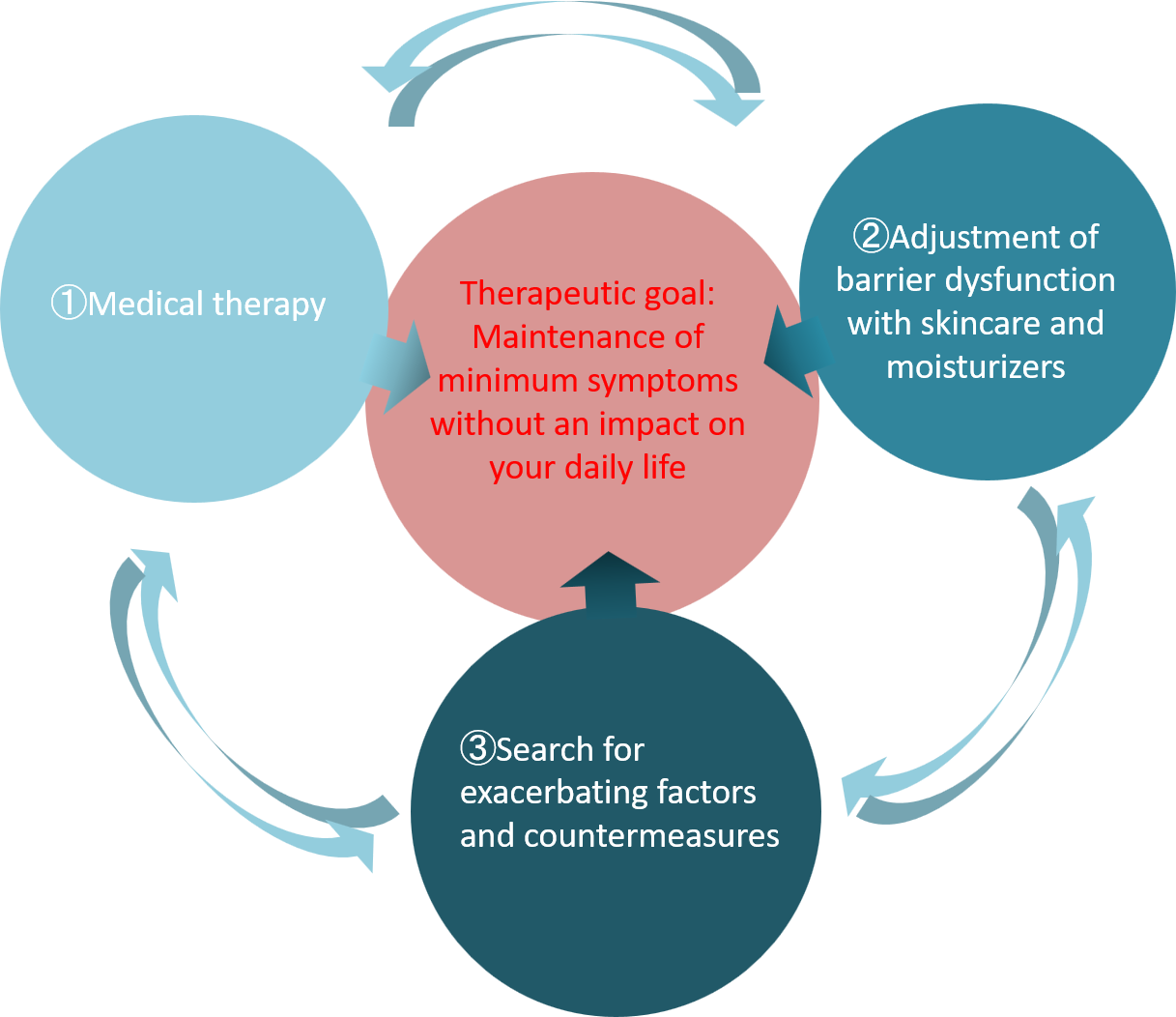
In order to achieve this, ① Medical therapy, ② Adjustment of skin barrier dysfunction with skincare and moisturizers, and ③ Searching for exacerbating factors and countermeasures should be combined and practiced in accordance with the severity and background of the individual patient’s eczema (Figure 4).
In order to achieve this, ① Medical therapy, ② Adjustment of skin barrier dysfunction with skincare and moisturizers, and ③ Searching for exacerbating factors and countermeasures should be combined and practiced in accordance with the severity and background of the individual patient’s eczema (Figure 4).
①Pharmacotherapy
1. Topical anti-inflammatory medications
Topical application of anti-inflammatory medication in most cases starts with topical steroid. There are other types of topical anti-inflammatory medications: Protopic® (generic name: tacrolimus), Corectim® (generic name: delgocitinib), and Moizerto® (generic name: difamilast). Once improvements of skin rashes are observed after topical steroid introduction, the alternative medications mentioned above can be used to keep the symptoms under control. We intend to select the strength and types of anti-inflammatory medications based on the extent of the eruption, or extent of improvement.
Topical application of anti-inflammatory medication in most cases starts with topical steroid. There are other types of topical anti-inflammatory medications: Protopic® (generic name: tacrolimus), Corectim® (generic name: delgocitinib), and Moizerto® (generic name: difamilast). Once improvements of skin rashes are observed after topical steroid introduction, the alternative medications mentioned above can be used to keep the symptoms under control. We intend to select the strength and types of anti-inflammatory medications based on the extent of the eruption, or extent of improvement.

2. Proactive application and reactive application
Initially, intensive topical anti-inflammatory medications including topical steroid are introduced to achieve a symptom-free state (remission introduction). Once remission is reached, there are two major therapeutic approaches thereafter.
The first approach is called ‘reactive application’ where intensive topical anti-inflammatory medication is applied every time you have a flare-up of eruptions, and once remission is obtained, topical medication is suspended (Figure 5).
Another approach is called ‘proactive application’ in which you keep applying the topical medication even after remission is reached just by reducing the frequency of application to three times a week or twice a week instead of completely stopping the topical application in order to maintain the remission (Figure 6).
We, at the clinic, advise on how to keep the symptoms under control through ‘proactive application’ once the remission is reached.
Initially, intensive topical anti-inflammatory medications including topical steroid are introduced to achieve a symptom-free state (remission introduction). Once remission is reached, there are two major therapeutic approaches thereafter.
The first approach is called ‘reactive application’ where intensive topical anti-inflammatory medication is applied every time you have a flare-up of eruptions, and once remission is obtained, topical medication is suspended (Figure 5).
Another approach is called ‘proactive application’ in which you keep applying the topical medication even after remission is reached just by reducing the frequency of application to three times a week or twice a week instead of completely stopping the topical application in order to maintain the remission (Figure 6).
We, at the clinic, advise on how to keep the symptoms under control through ‘proactive application’ once the remission is reached.
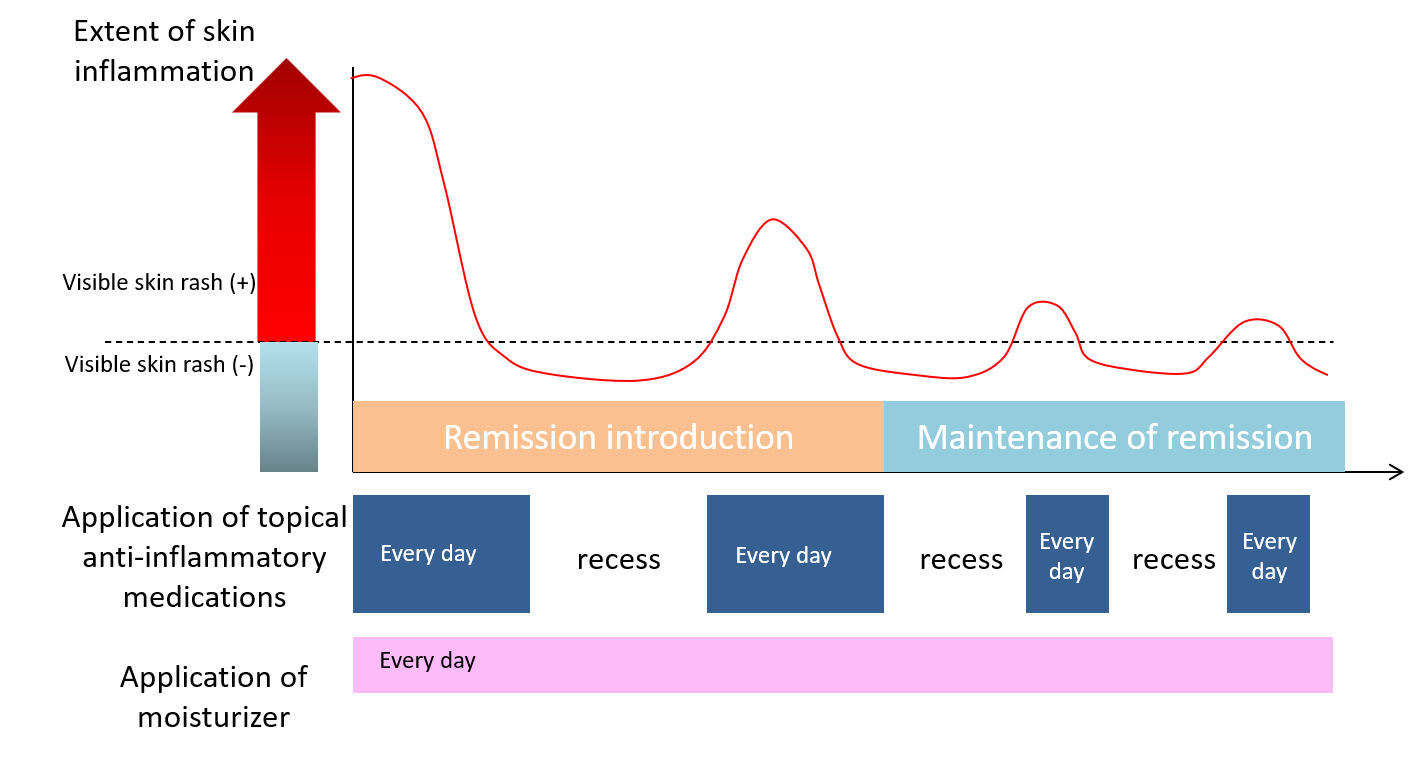
Figure 5. Reactive application: intensive topical anti-inflammatory medication is applied every time you have a flare of eruptions
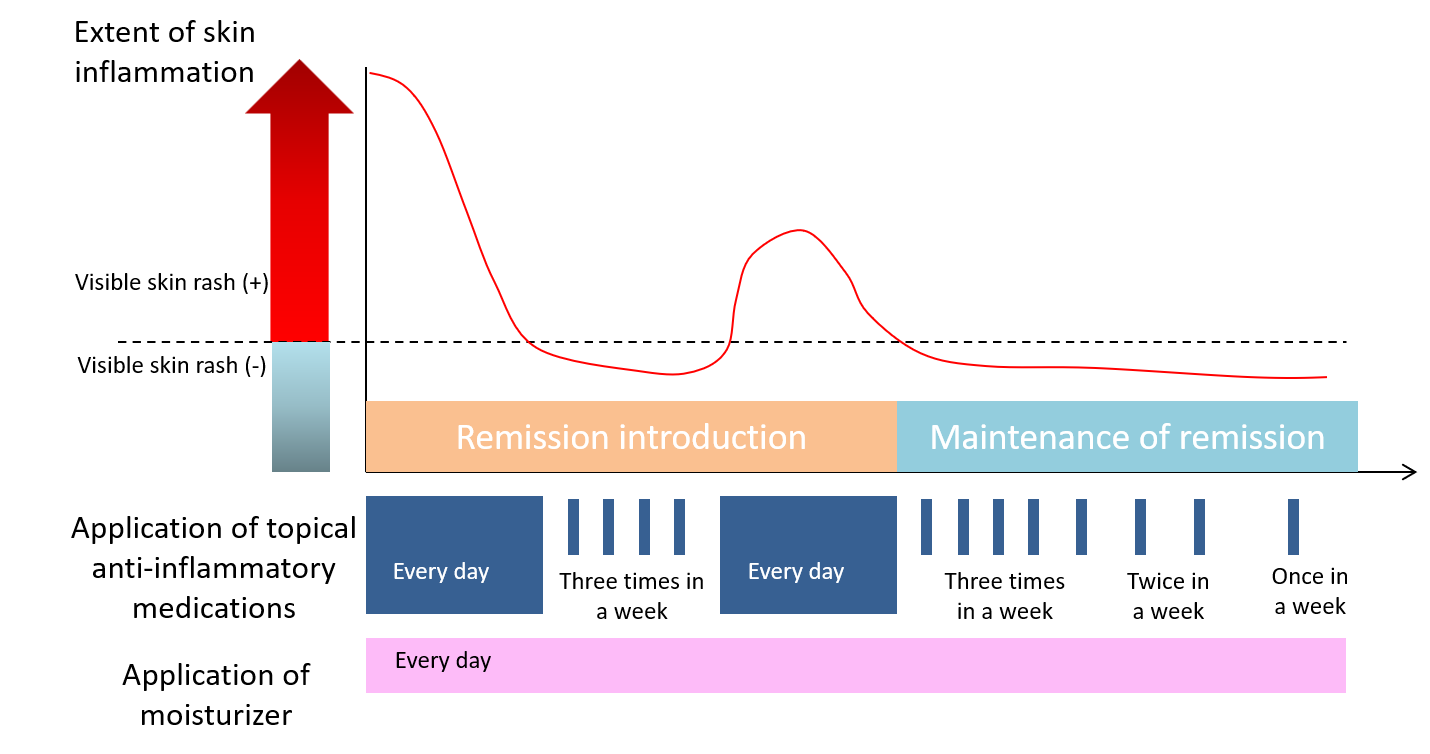
Figure 6. Proactive application: you keep applying the topical medication on a regular basis even after remission is reached
3. Control of itchiness by antihistamines
Antihistamines are oral medications that help reduce itchiness.
Although effectiveness varies from patient to patient, antihistamines are often effective adjunctive therapy in addition to topical treatments, such as anti-inflammatory medications and moisturizers.
Antihistamines are oral medications that help reduce itchiness.
Although effectiveness varies from patient to patient, antihistamines are often effective adjunctive therapy in addition to topical treatments, such as anti-inflammatory medications and moisturizers.
4. Systemic treatment for eczema
If you have recalcitrant, relatively severe symptoms of eczema (atopic dermatitis) whose skin manifestations do not improve despite intensive topical therapy, appropriate skin care, under certain conditions, systemic therapy may be applied. The progress in the systemic therapy has been remarkable in recent years, and the treatment of eczema is about to change, with a series of injectable and oral medications being newly approved, including DUPIXENT® (dupilumab), an injectable medication approved in 2018.
If you have recalcitrant, relatively severe symptoms of eczema (atopic dermatitis) whose skin manifestations do not improve despite intensive topical therapy, appropriate skin care, under certain conditions, systemic therapy may be applied. The progress in the systemic therapy has been remarkable in recent years, and the treatment of eczema is about to change, with a series of injectable and oral medications being newly approved, including DUPIXENT® (dupilumab), an injectable medication approved in 2018.
♦Injectable Treatments (Biological Drugs)
The injectable medications for eczema, DUPIXENT® (dupilumab), and MITCHGA® (nemolizumab) are categorized as ‘biological drugs’. Their generic name in parentheses both ends with ‘mab’, standing for ‘monoclonal antibody’, meaning that these are antibody drugs. Biological drugs, also known as biologics or biological agents are pharmaceutical drugs made from living sources or its products.
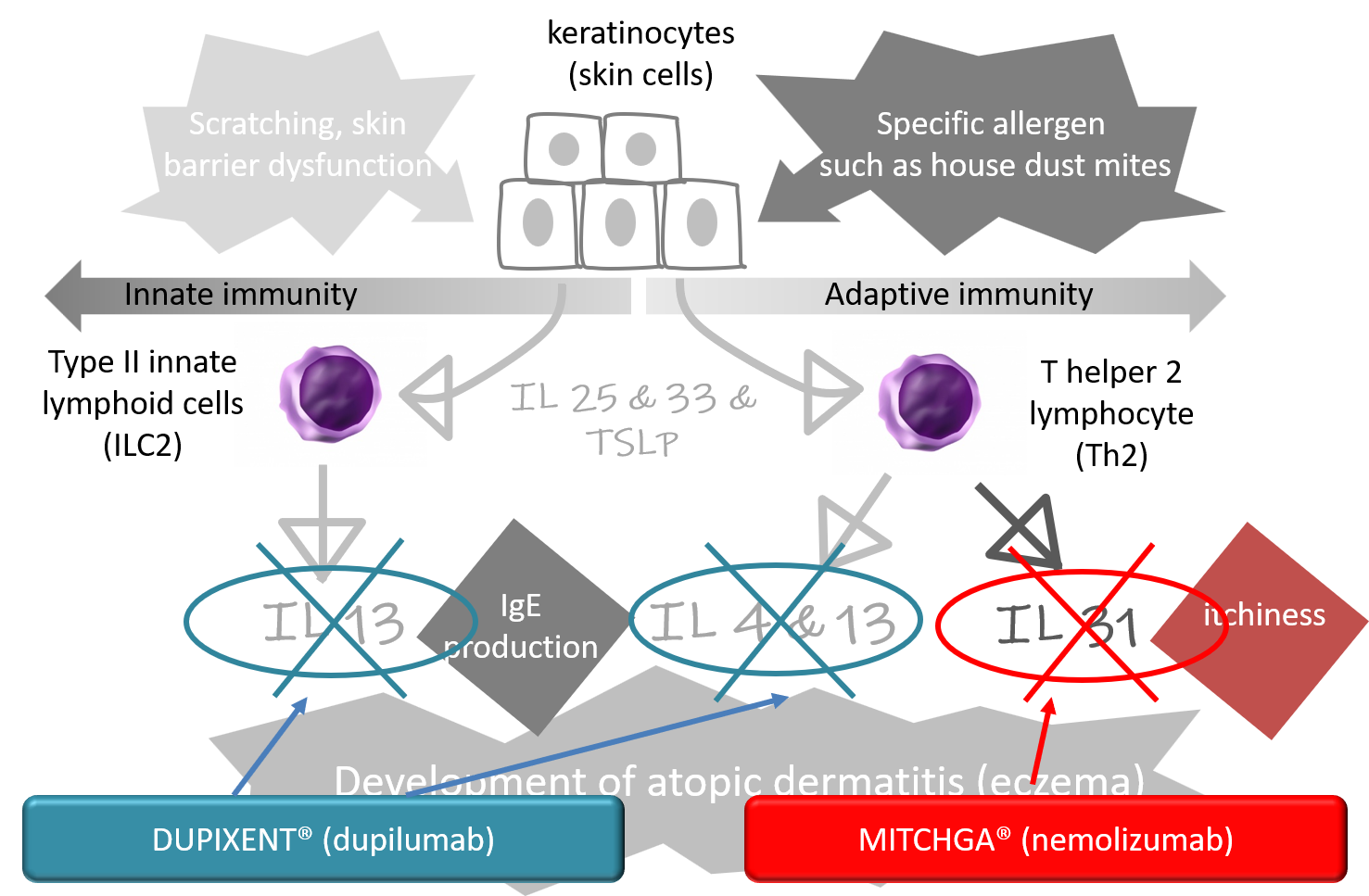
DUPIXENT® exerts its effect by blocking IL4 and IL13, whereas MITCHGA® reduces mainly itchiness by blocking IL31 (Figure 7). Patients on DUPIXENT® receive injections every two week, while one on MITCHGA® every four weeks.
ADTRALZA® or ADBRY (US) (tralokinumab) was newly approved as an injectable medication for eczema in December 2022 in Japan.
Systemic treatment for eczema including injections can be rather costly, and `High -Cost Medical Expense Benefit’ may apply to cover part of your medical expense if you have health insurance coverage in Japan and meet certain conditions.
The injectable medications for eczema, DUPIXENT® (dupilumab), and MITCHGA® (nemolizumab) are categorized as ‘biological drugs’. Their generic name in parentheses both ends with ‘mab’, standing for ‘monoclonal antibody’, meaning that these are antibody drugs. Biological drugs, also known as biologics or biological agents are pharmaceutical drugs made from living sources or its products.
DUPIXENT® exerts its effect by blocking IL4 and IL13, whereas MITCHGA® reduces mainly itchiness by blocking IL31 (Figure 7). Patients on DUPIXENT® receive injections every two week, while one on MITCHGA® every four weeks.
ADTRALZA® or ADBRY (US) (tralokinumab) was newly approved as an injectable medication for eczema in December 2022 in Japan.
Systemic treatment for eczema including injections can be rather costly, and `High -Cost Medical Expense Benefit’ may apply to cover part of your medical expense if you have health insurance coverage in Japan and meet certain conditions.

♦Treatments with oral medications
Novel oral medications for eczema treatment include JAK (Janus Kinase) inhibitors. JAK is a family of intracellular substances which promote the inflammatory process through the stimuli from cytokines such as IL4 and IL13. By preventing JAK activity, JAK inhibitor exerts its action in the treatment of eczema.
Another oral medication, NEORAL® (cyclosporine), is an immunosuppressant, with a longer history of use in the treatment of eczema.
As JAK inhibitors, OLUMIANT® (baricitinib), RINVOQ® (upadacitinib), and CIBINQO® (abrocitinib) can be the choices for moderate to severe eczema that is resistant to topical therapy in Japan. For the introduction of these JAK inhibitors, chest x-rays or chest CT scans, and blood tests are required in advance. Chest x-rays or chest CT scans must be done at the affiliated hospitals.
Systemic treatment for eczema including JAK inhibitors can be rather costly, and `High -Cost Medical Expense Benefit’ may apply to cover part of your medical expense if you have health insurance coverage in Japan and meet certain conditions.
NEORAL® can be administered for up to 3 months depending on its efficacy, with blood pressure measurements and blood tests to check drug concentration in the blood.
Novel oral medications for eczema treatment include JAK (Janus Kinase) inhibitors. JAK is a family of intracellular substances which promote the inflammatory process through the stimuli from cytokines such as IL4 and IL13. By preventing JAK activity, JAK inhibitor exerts its action in the treatment of eczema.
Another oral medication, NEORAL® (cyclosporine), is an immunosuppressant, with a longer history of use in the treatment of eczema.
As JAK inhibitors, OLUMIANT® (baricitinib), RINVOQ® (upadacitinib), and CIBINQO® (abrocitinib) can be the choices for moderate to severe eczema that is resistant to topical therapy in Japan. For the introduction of these JAK inhibitors, chest x-rays or chest CT scans, and blood tests are required in advance. Chest x-rays or chest CT scans must be done at the affiliated hospitals.
Systemic treatment for eczema including JAK inhibitors can be rather costly, and `High -Cost Medical Expense Benefit’ may apply to cover part of your medical expense if you have health insurance coverage in Japan and meet certain conditions.
NEORAL® can be administered for up to 3 months depending on its efficacy, with blood pressure measurements and blood tests to check drug concentration in the blood.
②Adjustment of skin barrier dysfunction with skincare and moisturizers
In eczema, dryness of skin is evident because of the disability to retain appropriate moisture due to barrier dysfunction. Also the barrier dysfunction makes the skin vulnerable to the external pathogens or allergens resulting in skin inflammation (figure 2).
Adjusting this barrier function by topical application of moisturizers or emollients is important to restore and maintain the skin barrier function.
Since external pathogens, allergens, and bodily fluids such as sweat on the skin can cause skin inflammation, it is important to keep the skin clean and inflammation-free by taking a shower.
Adjusting this barrier function by topical application of moisturizers or emollients is important to restore and maintain the skin barrier function.
Since external pathogens, allergens, and bodily fluids such as sweat on the skin can cause skin inflammation, it is important to keep the skin clean and inflammation-free by taking a shower.